|
|
The Overlooked Cause of DVT and Leg Pain
May-Thurner Syndrome (MTS) is a vascular condition that doesn’t always get the attention it deserves—but it should. While often underdiagnosed, MTS is a serious anatomical issue that can lead to chronic leg pain, swelling, and even dangerous blood clots like deep vein thrombosis (DVT).
At the Vascular Institute of Chattanooga (VIC), we’re committed to raising awareness and providing advanced diagnostic and treatment options for patients suffering from MTS. If you’ve experienced unexplained leg symptoms, recurring DVT, or venous insufficiency on the left side, May-Thurner Syndrome could be the hidden cause.
Let’s break down what May-Thurner Syndrome is, who it affects, how it’s diagnosed, and how VIC can help.
What Is May-Thurner Syndrome?
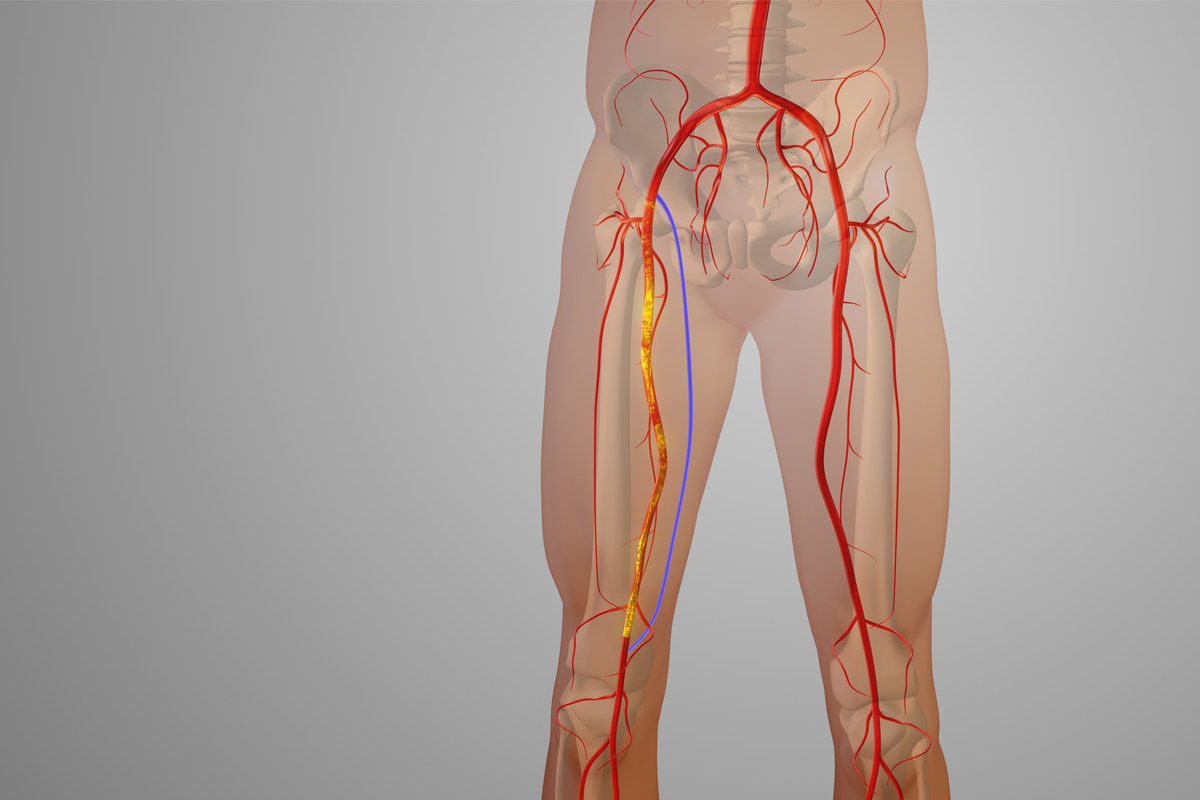
May-Thurner Syndrome occurs when the right iliac artery compresses the left iliac vein, which is the large vein that drains blood from your left leg. This anatomical “pinch” disrupts normal blood flow and increases the risk of blood pooling, clotting, and damage to the vein wall.
Over time, this can lead to the development of deep vein thrombosis (DVT), a blood clot that forms in a deep vein—most commonly in the left leg.
While MTS can occur in men and women, it’s more commonly diagnosed in women between the ages of 20 and 50, especially those who have experienced multiple pregnancies or have a history of venous issues.
Why It Matters: The Risk of DVT
The most serious complication of May-Thurner Syndrome is DVT. When blood flow is restricted in the left iliac vein, pressure builds and clot formation becomes more likely. DVT itself can be dangerous—causing leg pain, swelling, and discomfort—but the real danger is when a clot dislodges and travels to the lungs, resulting in a pulmonary embolism (PE), which can be fatal.
MTS is estimated to contribute to 20–30% of all left-sided DVT cases, yet it often goes unrecognized. That’s why identifying and addressing the underlying anatomical issue is so important.
Signs and Symptoms of May-Thurner Syndrome
Not everyone with May-Thurner Syndrome experiences symptoms right away. Some individuals live with it for years without knowing they have it—until they suffer a DVT or develop chronic venous issues.
When symptoms do occur, they often include:
- Unilateral swelling in the left leg
- A feeling of heaviness or tightness in the leg
- Pain, cramping, or aching in the leg—especially after prolonged standing
- Visible varicose veins in the groin or upper thigh
- Recurring DVT in the left leg
- Skin discoloration or ulcers in advanced stages
If you’ve experienced one or more of these symptoms, especially on the left side, it’s time to explore whether MTS may be the underlying cause.
How Is May-Thurner Syndrome Diagnosed?
At the Vascular Institute of Chattanooga, we use a multi-modality imaging approach to detect and confirm May-Thurner Syndrome. Because the compression occurs deep in the pelvis, it isn’t always visible with basic imaging techniques alone.
Diagnostic tools may include:
🩺 Venous Duplex Ultrasound
This non-invasive scan uses sound waves to evaluate blood flow in the leg veins. While helpful for identifying clots and reflux, it may not always detect compression in the pelvis.
🩻 CT or MR Venography
These advanced imaging tests provide detailed 3D views of the pelvic veins and arteries. They can detect narrowing or compression and are useful for surgical planning.
📌 Intravascular Ultrasound (IVUS)
Considered the gold standard for diagnosing MTS, IVUS allows for real-time internal imaging of the vein during a catheter-based procedure. It measures vein diameter, identifies areas of narrowing, and helps determine the need for treatment.
🩹 Venography
During this minimally invasive test, contrast dye is injected into the vein and X-ray imaging is used to map out blood flow. It’s often performed during interventional procedures for both diagnosis and treatment planning.
Treatment Options at VIC
If you are diagnosed with May-Thurner Syndrome, the goal of treatment is to restore proper blood flow, relieve symptoms, and prevent future DVT events.
At VIC, we offer minimally invasive, catheter-based procedures that are performed in our outpatient vascular suite with little to no downtime.
Most common treatment:
Iliac Vein Stenting
A self-expanding stent is placed inside the compressed portion of the vein to hold it open and allow blood to flow freely. The procedure is typically done using IVUS and venography for precision and safety.
✅ No general anesthesia
✅ Same-day discharge
✅ Rapid symptom relief
✅ Return to normal activities in a few days
For patients with existing DVT, additional procedures such as thrombolysis (clot-dissolving medication) or mechanical thrombectomy may be performed to remove the clot before placing the stent.
Long-Term Outlook and Follow-Up

With timely diagnosis and proper treatment, most patients experience dramatic improvements in symptoms and quality of life. Our team at VIC follows a comprehensive post-procedure care plan that includes:
- Surveillance imaging to monitor stent function
- Compression therapy (if needed)
- Risk factor management
- Preventive measures for clotting (such as blood thinners or activity modifications)
We work closely with patients to ensure that treatment is effective—and lasting.
Why Choose the Vascular Institute of Chattanooga?
At VIC, we are proud to be the region’s premier destination for complex venous disease. Our board-certified vascular specialists combine compassionate care with the latest in diagnostic and interventional techniques to treat May-Thurner Syndrome effectively and efficiently.
🟢 Advanced imaging and diagnostics
🟢 On-site outpatient procedures
🟢 Same-day or next-day appointments
🟢 Patient-focused care that listens and acts
If you’re dealing with unexplained leg pain, swelling, or have a history of DVT, don’t wait—ask us if May-Thurner Syndrome could be the cause.
Take the next step toward relief.
📍 Schedule your vein consultation today
📞 Call VIC to book a same-day appointment
🌐 Visit www.vascularinstituteofchattanooga.com for more information