A common complication of post-thrombotic syndrome can occur in patients after experiencing a Deep Vein Thrombosis (DVT). The small valves found inside the veins in the arms and legs allow/help the blood to flow properly in the body. If a DVT occurs, the clot/blockage can damage the valves, preventing proper blood flow from happening.
The valves in your veins are responsible for making sure the blood is flowing toward the heart. However, reflux can occur when the blood flows in the opposite direction because of the damaged valves. This abnormal flow causes discomfort, swelling, and skin damage in patients.
If you are experiencing these signs/symptoms and have had a DVT, listen to your body and be evaluated.
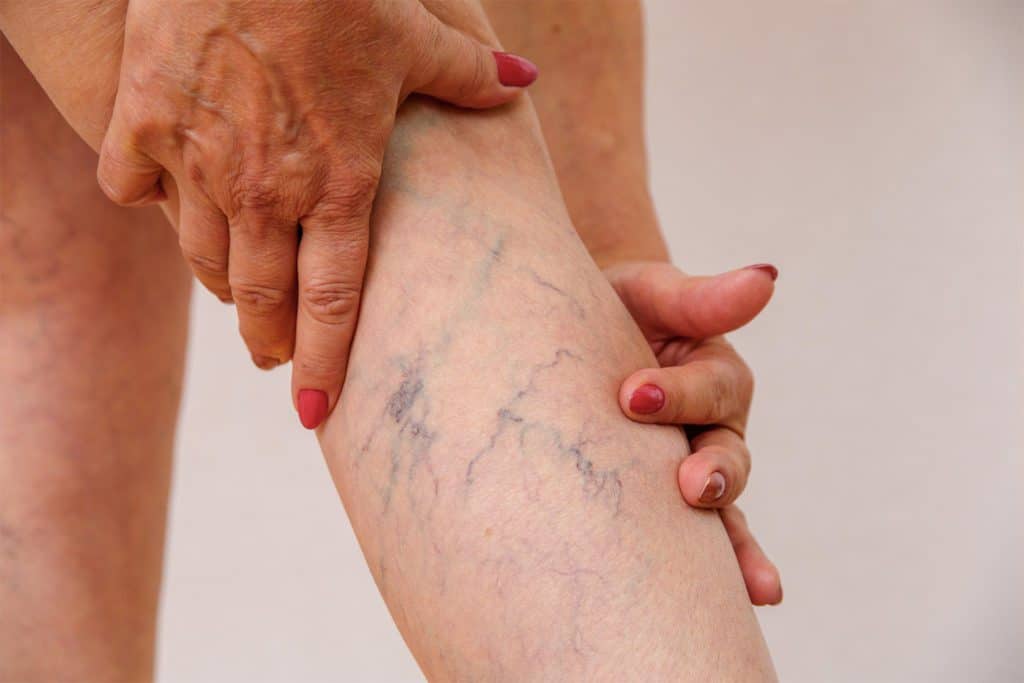
You Have a Choice When It Comes to Vascular Care.
Get an Appointment at VIC In 1 to 3 days – Without a Referral!
You Have a Choice When It Comes to Vascular Care.
Get an Appointment at VIC In 1 to 3 days – Without a Referral!
In patients who show the signs of chronic venous insufficiency, swelling of the leg and skin changes, or who have had known DVT, a vascular specialist exam is required to stage the disease process. Often an ultrasound would be performed to detect chronic DVT or valvular dysfunction. Preventive measures for vein and skin health would be recommended.

While the condition cannot be reversed, it can be managed with lifestyle changes. The progression of the disease will lead to discomfort, itchiness, and redness of the skin on the legs. Pressure in the legs worsens over time, and the vein walls and valves are affected, limiting the blood flow and making it a true mobility problem for some. Venous ulcers or sores can form at the ankle area and can be very difficult to treat.
Living with PTS can be challenging as it’s a condition that doesn’t entirely disappear. However, it is manageable through lifestyle choices, compression hose, and sometimes treatment with medication.
Yes, complications of PTS can include leg ulcers and wounds, which require monitoring by a wound care specialist. If these wounds aren’t properly managed, they can worsen, potentially leading to surgical intervention.
Always listen to your body. If you notice increasing pain, a new ulcer on your leg, signs of infection in an existing ulcer, increased swelling, or heaviness in your legs, these are post thrombotic syndrome symptoms that warrant contacting your provider for evaluation and to prevent further damage.
Experiencing varicose veins, spider veins, chronic venous insufficiency, or leg swelling?
The Vascular Institute of Chattanooga provides advanced, minimally invasive treatments including:
• Endovenous ablation
• Venaseal™ vein closure
• Radiofrequency therapy
• Sclerotherapy
• Deep venous evaluation
✔ No referral required
✔ Same-week appointments
✔ Insurance accepted
✔ Only nationally accredited deep venous center in the region
After medical treatment, patients may enhance cosmetic results through our partnership with Alchemy MedSpa.
New clients receive 10% OFF aesthetic services when mentioning this ad.
Comprehensive vein health + aesthetic refinement — all in Chattanooga.
Call now to book an appointment.
Conveniently located near Northgate Mall.